Tackling Corneal Blindness and Building Systems in Sierra Leone

This spring, I had the opportunity to travel to Freetown, Sierra Leone to participate in a corneal transplant partnership established over five years ago between Dr. Lloyd B. Williams and Dr. Lloyd H. Williams—yes, that’s “Dr. Lloyd Williams squared!” Their collaboration began serendipitously at the American Academy of Ophthalmology meeting in 2020, and it’s hard not to feel that something like fate brought them together. Since then, the team has completed seven trips, performing and teaching more than 120 corneal transplants and I felt incredibly fortunate to join the most recent mission.
After nearly 24 hours of travel, we arrived in Sierra Leone’s Lungi International Airport, followed by a 45-minute ferry ride across the Sierra Leone River into Freetown. The city is vibrant and bustling—filled with zigzagging tricycles (“kekes”), pedestrians balancing impressively large loads on their heads, and street vendors selling everything from coconuts to imitation sunglasses.
Upon arriving at Connaught Hospital, we began with a full day of screening nearly 60 pre-selected patients with corneal blindness. Their conditions ranged from infectious and traumatic corneal scarring to keratoconus and pseudophakic bullous keratopathy. Determining surgical candidates felt like a complex game of Tetris—carefully matching a limited number of donor corneas to patients based on age, severity of vision loss, and likelihood of success. I kept a running list of potential candidates throughout the day, and by evening, we finalized a surgical schedule for the days ahead.
We also had the chance to evaluate postoperative patients from prior trips, including the very first corneal transplant recipient in Sierra Leone from over five years ago. I had only seen photos of her before, so meeting her in person and witnessing the impact of her surgery was especially meaningful.
Over the next three days, we operated on two tables, completing 4–6 cases daily. Performing surgery in this setting presents unique challenges: older microscopes, variable instruments, minimal anesthesia, and higher stakes, as many patients may not have another opportunity for another surgery. Despite this, the operating room team—nurses and technicians alike—were exceptional. We worked efficiently and maintained high spirits, with good music playing in the background.
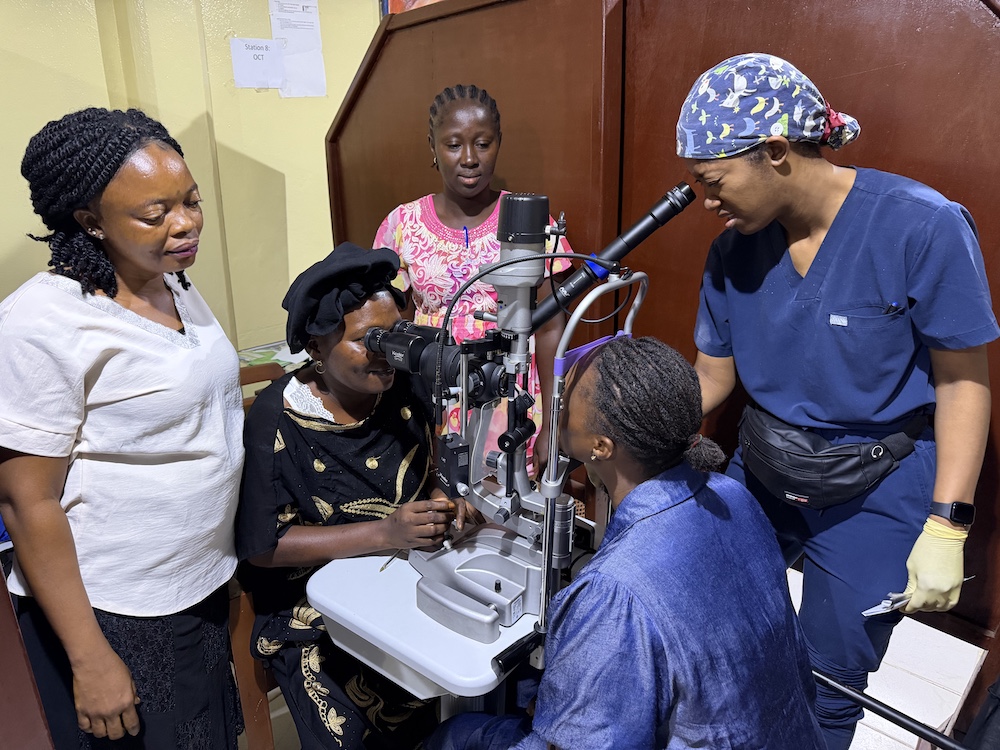
Each morning, we rounded on postoperative patients alongside the local team. Remarkably, every patient returned for their first follow-up visit—a testament to thoughtful preoperative counseling and patient education about the importance of postoperative care. During clinic time, we also worked closely with ophthalmic nurses who were eager to learn foundational skills, from checking visual acuity to using the slit lamp. The need for basic training is immense, and even small teaching efforts can have a lasting impact here.
Follow-up beyond the early postoperative period remains a major challenge. As Sierra Leone’s Dr. Williams explained, most patients return on postoperative day one, sometimes at one month, but many are eventually lost to follow-up. When I asked Dr. Williams about this, he offered an encouraging perspective: “The reason most people don’t return is because they are doing well. I guarantee you that those you are seeing here are back because they are having a problem.”
Sierra Leone is one of the world’s poorest countries, and access to healthcare remains very limited. In conversations with Dr. Lloyd H. Williams, I learned that there are currently only six practicing ophthalmologists in the country—and just three who perform surgery—equating to approximately 0.5 surgical ophthalmologists per million people. In contrast, the United States has roughly 20 ophthalmologists per million. The resulting surgical backlog is enormous, and the need for training is urgent. Despite these challenges, I was deeply impressed by the progress being made, driven by extraordinary leaders like Dr. Lloyd H Williams and Dr. Jalikatu Mustapha.
One of the most exciting developments this year was the launch of an ophthalmology residency program at Connaught Hospital. The program welcomed its first two residents this year, marking a critical step toward sustainable, local capacity-building. I had the pleasure of working with one of the PGY-1 residents, Andrieu Sannoh, whose enthusiasm and eagerness to learn was truly inspiring.
My time in Sierra Leone reinforced for me that sustainable impact in global ophthalmology lies not only in the surgeries we perform, but in the partnerships we build and the systems we help strengthen. I look forward to returning to Sierra Leone and continuing to build meaningful collaborations.