THE GLAUCOMA DIVISION AT DUKE STANDS AMONG THE BEST IN THE WORLD — by size and reputation. It is one of the largest glaucoma programs in the U.S. and ranks among the top five globally for research, education, and patient care. “We are a triple threat,” said Leon W. Herndon Jr, MD, professor of ophthalmology and and glaucoma division chief. “I trained at Duke under the direction of the first Chief of the Glaucoma Division, M. Bruce Shields, MD over 30 years ago, and have witnessed tremendous growth of our program over the years.”

A Growing Global Challenge
Glaucoma, the leading cause of irreversible blindness, affects roughly 80 million people worldwide, including four million Americans. Caused by optic nerve damage, often linked to high intraocular pressure, its origins remain unclear. Some patients develop glaucoma despite normal eye pressure. While there is no cure, early detection and treatment can slow progression, making timely diagnosis critical.
With expert faculty, accomplished fellows, and a skilled staff, Duke’s glaucoma program is outstanding by any standard. Herndon and W. Daniel Stamer, PhD, Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology and vice chair for research, aim to elevate this excellence further by establishing the Duke Glaucoma Center of Excellence — a philanthropic initiative to expand and sustain the program’s impact.
“We have the infrastructure, patients, and personnel, with a long history of excellence,” Herndon said. “An endowed center will provide critical resources and flexibility to keep innovating.”
The timing is urgent. Glaucoma prevalence rises with age, and the aging population signals an impending surge in vision-related diseases. “The disease can begin decades before symptoms appear. Half of those with glaucoma don’t know they have it until they notice vision loss,” Stamer said. Meanwhile, federal research funding and insurance reimbursements are shrinking, making private support essential.
A Foundation of Collaboration
The collaborative culture at Duke is a cornerstone of its success. “When clinicians and scientists come together, ideas flourish,” Herndon said. This synergy began under David Epstein, MD, former ophthalmology chair and glaucoma specialist, who championed physician-scientist partnerships. Today, Duke boasts 17 physicians and basic science faculty, a critical mass of experts exploring glaucoma from multiple angles.
Katy Liu, MD, PhD, who completed both clinical and research fellowship training at Duke before joining the faculty, calls the interaction between clinicians and researchers unique. “There’s constant cross-talk between the lab and clinic,” she said.
Seeking Better Treatments Through Research
Duke’s reputation for cutting-edge research drew Liu to the program. Her work investigates how immune cells, particularly macrophages, may disrupt the eye’s drainage system, raising pressure and increasing glaucoma risk. Her goal is to develop a therapy to target immune pathways that lower eye pressure.
Glaucoma researchers at Duke are pushing beyond today’s treatments to uncover how pressure, genetics, and cellular stress drive vision loss. In Stamer’s lab, advanced gene profiling is helping identify the specific genes and cell types involved in glaucoma, opening the door to more precise, targeted therapies.
Meanwhile, research led by Paloma Liton, PhD, professor of ophthalmology, is exploring how stress alters the eye’s drainage system and how those changes may set the stage for disease. Together, these discoveries are helping move the field from basic science toward better diagnostics, improved treatments to control eye pressure, and new strategies to preserve sight.
Collaborating with Columbia University, Stamer is mapping gene expression in cells that regulate eye pressure — a step toward precision therapies.
Research led by Vasantha Rao, PhD, Richard and Kit Barkhouser Distinguished Professor of Ophthalmology, in collaboration with Epstein, identified Rho kinase as a novel therapeutic target for lowering intraocular pressure. Their work demonstrated that inhibiting Rho kinase improves fluid outflow through the trabecular meshwork — a breakthrough that paved the way for Rhopressa, a first-in-class glaucoma medication and the first FDA-approved glaucoma therapy in over 20 years. This discovery underscores Duke’s role in translating science into sight-saving treatments.
Educating Future Leaders
Education is central to Duke’s mission. The division trains five clinical fellows annually and up to four research fellows and post-docs — more than any other U.S. glaucoma fellowship program. “We attract superb fellows,” Stamer said. “They are our legacy.”
Herndon credits former glaucoma chief R. Rand Allingham, MD, for instilling this focus. “He believed Duke fellows receive the best training, so let’s send as many as possible into the field.” Herndon said. These graduates carry Duke expertise across the globe, advancing care and research for decades to come.
Patient Care: The Heart of It All
Every effort — research, training, collaboration — ultimately serves one purpose: exceptional patient care. Duke glaucoma specialists take care of almost 50,000 patient visits each year.
“If my mom had glaucoma, I’d fly her from California to Duke,” Stamer said. “She’d get the best care here.” Duke is equipped to handle the most complex cases, attracting patients from across the Southeast.
“We can offer every available glaucoma treatment,” Liu said. A center of excellence would strengthen this foundation, ensuring continued world-class care and accelerating progress toward a cure.
The goal is simple. Provide the best possible glaucoma care to the most patients we can. A center of excellence would take the Duke Glaucoma Division to the next level.
Help Us Shape the Future
Duke’s Glaucoma Division is poised to shape the future of glaucoma care worldwide — through research, education, and patient care. With philanthropic support, the vision of a Center of Excellence will secure this legacy and ensure that innovation and excellence will endure.
Meet the Duke Glaucoma Faculty
Immune Cells Play Key Role in Regulating Eye Pressure Linked to Glaucoma
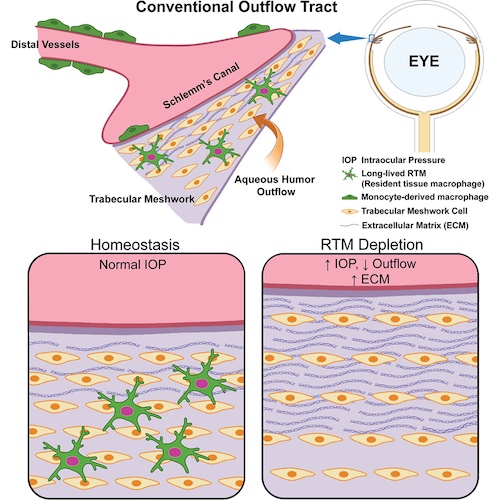
A new study published in Immunity uncovers a surprising player in preventing glaucoma: the eye’s own immune cells. Researchers at Duke University School of Medicine have identified resident macrophages — specialized immune cells that live within the eye’s drainage tissues — as essential for keeping eye pressure in check.
When the eye’s drainage system clogs, pressure builds up and causes damage. The pressure can lead to glaucoma and vision loss. Until now, the role of these resident macrophages in that process had been unclear.
“The only way we can treat glaucoma is by lowering the eye pressure, yet we still have patients who go blind despite current treatments,” said Katy Liu, MD, PhD, lead author and assistant professor of ophthalmology. “This research helps us understand the role of the immune system in regulating eye pressure.”
Using fluorescent tagging in animal models, the team observed resident macrophages at work. When the cells were selectively removed, the eye’s drainage pathways clogged, fluid accumulated, and pressure rose. “Our findings show that resident macrophages are essential for maintaining healthy eye pressure,” Liu said. “Disruption of this system may contribute directly to the development of glaucoma.”
The discovery opens the door to therapies that target these cells directly — an entirely new direction for glaucoma treatment. “Now we have a specific target for developing new therapies that can normalize the eye pressure and stop vision loss, in contrast to current medications that do not target the source of disease,” said W. Daniel Stamer, PhD, corresponding author and Joseph A.C. Wadsworth Distinguished Professor of Ophthalmology.
This work builds on Duke Eye Center’s long history of translating lab discoveries into real world treatments, including the first FDA approved glaucoma drug in two decades. “This discovery is a major step forward in understanding how the immune system contributes to the regulation of eye pressure,” said Daniel Saban, PhD, co-corresponding author. “This research builds on Duke’s strong history of turning laboratory findings into real treatments for patients.”
In addition to Liu, Saban and Stamer, study authors include Aleksander O. Grimsrud, Maria Fernanda Suarez, Darren Schuman, Michael L. De Ieso, Megan Kuhn, Ruth A. Kelly, Rose Mathew, Joan Kalnitsky, Matthias Mack, Gerasimos Anagnostopoulos, Florent Ginhoux, Violet Bupp- Chickering, Revathi Balasubramanian, and Simon W. M. John.
The study is funded by the National Institutes of Health (K08EY032202), Research to Prevent Blindness, the Duke Strong Start Award, the Heed Fellowship and the American Glaucoma Society.